Exceptional Specialty Pet Care Close to Home
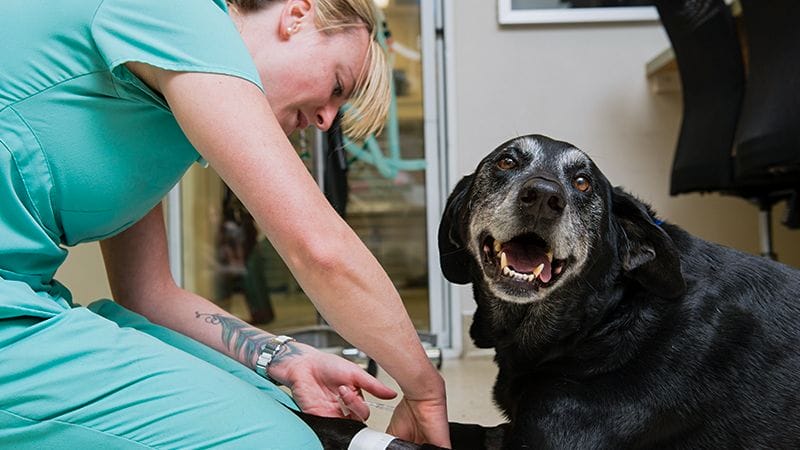
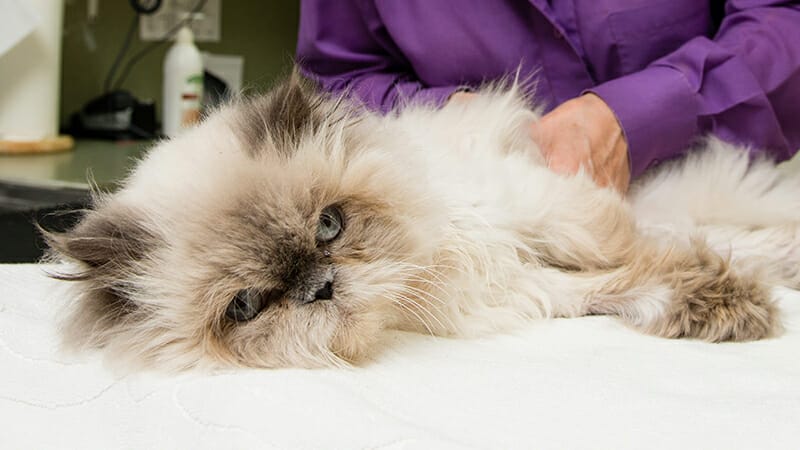
Your pet is a part of your family, and we understand that facing a medical difficulty can be stressful. You can rely on our compassionate, expert team to make the process as easy as possible.
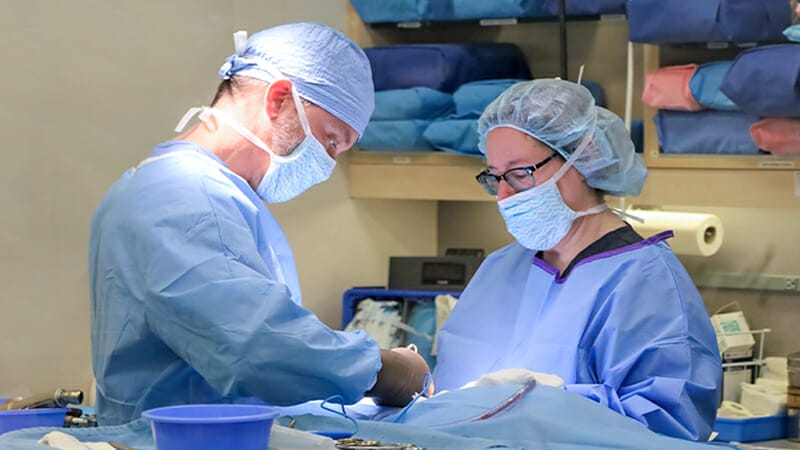
MedVet Houston Bay is a trusted partner in care for family veterinarians and pet lovers. As a referral-only specialty center, we work closely with your family veterinarian to provide your pet with diagnostic expertise, sophisticated imaging, specialized treatments and procedures, and 24-hour critical care. We work to deliver the best outcome for your pet, and you’ll get updates each step of the way to put your mind at ease.
Our team has the expertise and the resources in our state-of-the-art facility to diagnose and treat your pet, giving them the best chance for a longer, happy life.